coronavirus &COVID-19 &Vaccine Bill Brieger | 25 Aug 2022
COVID-19 Vaccine Hesitancy Is Rising In Ghana: Time To Take Action
Andaratu Wuni has contributed this posting to the Blog site for the JHU site for the course Social and Behavioral Foundations of Primary Health Care.
 (Graphic source: https://www.aafp.org/news/health-of-the-public/20210429vacchesitancy.html)
(Graphic source: https://www.aafp.org/news/health-of-the-public/20210429vacchesitancy.html)
Covid 19 has unarguably wrecked devastating consequences globally since its emergence and has proven to to be a ubiquitous public health health problem. Vaccination against the virus has been shown to be the most effective way of limiting severe disease and mortality. However the spate of vaccine hesitancy in Ghana has continued to rise in the last year. The World Health Organization defines vaccine hesitancy as the delay in acceptance or refusal of vaccination despite availability of vaccination services. This public health problem has far reaching consequences not only in Ghana but globally. Currently the vaccine hesitancy rate in Ghana is about 30% and counting! with people 25 years and under leading the hesitancy core.
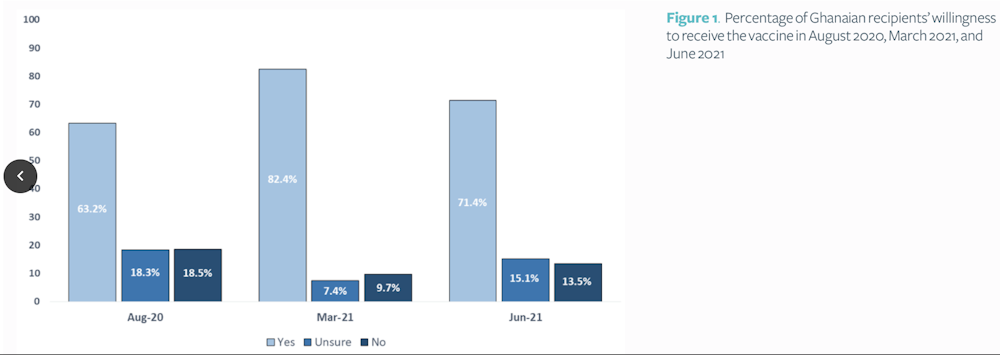
(Graph Source: https://figshare.com/articles/thesis/Examining_drivers_of_COVID-19_vaccine_hesitancy_in_Ghana/14494851)
Since Ghana rolled out vaccines to the general public over one year ago, only 25.9% of the population have been fully vaccinated as of August 19,2022.Ghana has a target of vaccinating 22.9million eligible Ghanaians; that is about 60% of the population in order to achieve herd immunity, however only 8.2 million Ghanaians have been fully vaccinated to date.
Many reasons account for the rise in covid 19 vaccine hesitancy in Ghana; from the depletion of rigorous and continuous education and the consequent lack of community engagement, relaxation of covid 19 protocols, to vaccine misinformation and conspiracy theories as well as political influence. It is time for a policy that will mitigate this crucial problem, which the WHO(before the covid pandemic) described as one of the top ten greatest threats to global health.
The truth is, a single policy may not totally solve the problem as the issue of vaccine hesitancy is a complex one. The best approach will be for policymakers to enact policies to make vaccination a condition for other essential services in Ghana.
Intensify mandatory vaccination especially in high risk individuals and high risk locations, eliminate vaccine exemptions based on all but health related reasons, commit to structured community engagements and outreaches using the key stakeholders like the Ghana Medical Association and the Public Health association of Ghana, use stakeholders like UNICEF Ghana and the Ghana Health Service to disseminate accurate and scientifically proven vaccine information and last but not least introduce incentives for citizens who take the vaccine.
Dengue &Vaccine Bill Brieger | 23 Aug 2022
Dengue vaccines in Singapore – a luxury or a necessity?
Edwin Chng has contributed this posting to the Blog site for the JHU site for the course Social and Behavioral Foundations of Primary Health Care.
 Dengue has been endemic in Singapore for many decades, with all four dengue serotypes (DENV-1-4) in active circulation. It presents a significant impact on the economy, with the financial burden of dengue estimated to be US$1.04 billion from 2010 to 2020. (Mosquito Photo credit: http://bitly.ws/twG2)
Dengue has been endemic in Singapore for many decades, with all four dengue serotypes (DENV-1-4) in active circulation. It presents a significant impact on the economy, with the financial burden of dengue estimated to be US$1.04 billion from 2010 to 2020. (Mosquito Photo credit: http://bitly.ws/twG2)
Despite aggressive conventional vector control measures such as fogging and breeding site elimination, Singapore continues to have persistent outbreaks annually. The number of cases in recent years have also surged. From January to July 2022, 9 deaths and 22,468 cases have been reported thus far – the latter number is more than 4 times the number of cases reported in the whole of 2021. Dengue cases is likely to continue to increase, as the traditional peak dengue season in the country is from June to October each year. (Dengue Cases Graph Photo credit: NEA)
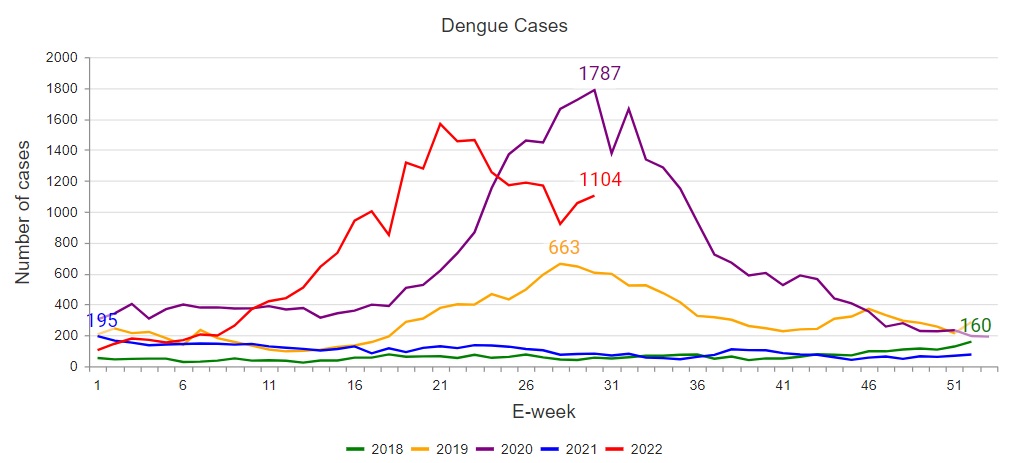
Singapore’s dengue crisis can be attributed to climate change and a recent change in the prevailing serotype. In the past, the dominant strains in Singapore were DENV-1 and DENV-2, hence the Singapore population has lower immunity to the other two strains. As a result, a large proportion of the population remains susceptible to DENV-3, which is emerging as the dominant strain in Singapore.
As such, as per the World Health Organization, dengue vaccination remains an integral part of dengue prevention and control strategy. The vaccine has an efficacy of about 80% against the outcomes of infection, hospitalization and severe infection which is potentially lethal. Unfortunately, the Singapore government has decided not to include it in the national immunization program, hence it is not eligible for government subsidy. As a result, the vaccine which costs a hefty USD450 remains inaccessible to the  average Singaporean. (Vaccine Photo credit: http://bitly.ws/twGk).
average Singaporean. (Vaccine Photo credit: http://bitly.ws/twGk).
Various stakeholders including the National Center for Infectious Diseases, primary care physicians and pharmaceutical companies can rally and work together in awareness campaigns and clinical studies. Health economics data from such collaborations can confirm the cost-effectiveness of dengue vaccines and positively influence the government to consider a change in its existing policy to provide subsidies. Increasing its accessibility and affordability to more Singaporeans will definitely contribute significantly to the fight against dengue in Singapore.
Cancer &Community &HPV &Vaccine Bill Brieger | 23 Aug 2022
Stop Cervical Cancer: Promote HPV Vaccination in Kenya
Lisa Marie Clark has contributed this posting to the Blog site for the JHU site for the course Social and Behavioral Foundations of Primary Health Care.
Cervical cancer is among the leading causes of death for Kenyan women. Every day, 9 women die from cervical cancer alone in Kenya. HPV vaccination reduces the risk dramatically, particularly for HPV types 16 and 18, which may be responsible for up to 70% of cervical cancers.
Optimal vaccination is in early adolescence starting at age 10, before sexual activity begins. In 2020, uptake of the HPV vaccine in Kenya was low, with only 33% of the target population receiving the first dose and only 16% percent receiving a second dose. Low uptake may be due to a variety of factors including misinformation, lack of access, and low supply of vaccines.
In 2019, the Kenyan Ministry of Health began including the HPV vaccine in the routine vaccination schedule. The vaccine, with support from GAVI, the vaccine alliance, is offered free of charge. However, the Catholic Church and medical professional groups influenced by religious ideology have been a major opponent to vaccine uptake. The Kenya Catholic Doctors’ Association has been vocal about urging parents to promote abstinence over vaccination, equating HPV vaccination with permission to engage in sexual activities. See vaccination from Republic of Kenya’s Ministry of Health in photo.
In the face of such obstacles to vaccine uptake, more funding is needed to strengthen Kenya’s vaccination campaign, with a focus on building trust and strengthening partnerships with faith leaders to improve vaccine uptake. With more funding from GAVI and improved community engagement vaccination rates would improve, HPV infection rates would decrease, and lives would be saved as a result.
coronavirus &Ebola &Vaccine Bill Brieger | 13 Jul 2022
Malaria and Tropical Health Update for 6-13 July 2022
Please see some excerpts from recent news/media reports on COVID-19, Malaria, Marburg Virus, Ebola, Microplastics and more. Follow links for full articles.
Channels TV reports that Nigeria has confirmed 357 new cases of COVID-19 amid the wave of fresh infections resurging in parts of the country. The number of new cases has continued to rise as authorities have yet to restore the relaxed measures initially put in place to curb the spread of the disease. In a tweet on Tuesday, the Nigeria Centre for Disease Control (NCDC) explained that the fresh infections were confirmed between July 9 and 11. These cases, it stated, were reported in five states and the Federal Capital Territory (FCT).
BioNTech to take malaria vaccine into clinical trials later this year as reported on 12-Jul-2022 By Rachel Arthur. BioNTech is readying to take its mRNA malaria vaccine candidates into clinical trials later this year.
Mzuzah Webinar on “The Effects of Microplastics on Human Health” on Tuesday, July 26, 2022 from 10:00 AM to 12:00 PM CDT. Mzuzah Africa is a multidimensional platform, which connects stakeholders from key sectors in the sustainability discourse. These dialogues are essential to ensure the development of Sustainable Leadership with highly skilled, right-thinking individuals leading the transformational movement in Africa.
Faced with COVID and monkeypox, new USAID leader draws strength from African proverb. From NPR July 11, 2022. Dr. Atul Gawande began a challenging new job this year. The surgeon, former New Yorker staff writer and bestselling author of books like Being Mortal: Medicine and What Matters in the End, is now the head of global health for the U.S. Agency for International Development, which provides foreign and humanitarian aid around the world. So far it’s been quite a daunting year. The pandemic has of course continued and cases are now surging in many countries. Then there’s the worldwide monkeypox outbreak, the potential global repercussions of the U.S. Supreme Court’s decision to overturn Roe v. Wade, and other health crises that have arisen in the wake of the pandemic. Gawande spoke to NPR about the agency’s top health priorities in low-income countries.
On July 11, 2022 Jessica Nye wrote that Ebola Reduces Visual Quality of Life in Pediatric Patients. Survivors of EVD and their close contacts were found to have poor health- and vision-related quality of life, especially among children with one or more ocular complications. Shantha JG, Canady D, Hartley C, et al. Ophthalmic sequelae and psychosocial impact in pediatric ebola survivors. EClinicalMedicine. 2022;49:101483. doi:10.1016/j.eclinm.2022.101483
The Express (UK) reported that Marburg Virus, an Ebola-like virus with 88% death rate has hit Ghana as fever sparks ‘serious concern’ AN OUTBREAK of a deadly virus similar to Ebola, called Marburg, has been identified in Ghana, as two people were diagnosed with the highly contagious disease after they had died. Vassia Barba wrote on Jul 8, 2022. The World Health Organization (WHO) said on Thursday “preparations for a possible outbreak response are being set up swiftly as further investigations are underway”. In a statement, the WHO said preliminary assessment of samples from the two patients indicate the cases were positive for Marburg. However, it clarified those results must be confirmed by a laboratory in Senegal.
FutureLearn is offering an online course, The Resistant Mosquito: Staying Ahead of the Game in the Fight against Malaria. Discover how we can keep the upper hand in our fight against the malaria mosquito by managing insecticide resistance development. This course will be available on FutureLearn from 25 July 2022. The link to the course will follow on July 25th.
Development &poverty &Vaccine Bill Brieger | 28 Apr 2022
African Immunization Week Press Briefing: Reducing Poverty, Saving Lives
 The World Health Organization’s African Regional Office held a press briefing to mark World Immunization Week/African Immunization Week. Three experts shared their observations of developments and trends and responded to questions over the course of an hour on Thursday 28th April. The panelists included Dr Benido Impouma, Director, Communicable and Noncommunicable Diseases, WHO Regional Office for Africa, Professor Helen Rees, Executive Director, Wits Reproductive Health and HIV Institute, University of Witwatersrand, South Africa, and Hon. Dr Kailash Jagutpal, Minister of Health and Wellness, Government of Mauritius. In addition, Dr. Mory Keita answered questions about the latest Ebola Virus Disease (EVD) in the Democratic Republic of the Congo (DRC).
The World Health Organization’s African Regional Office held a press briefing to mark World Immunization Week/African Immunization Week. Three experts shared their observations of developments and trends and responded to questions over the course of an hour on Thursday 28th April. The panelists included Dr Benido Impouma, Director, Communicable and Noncommunicable Diseases, WHO Regional Office for Africa, Professor Helen Rees, Executive Director, Wits Reproductive Health and HIV Institute, University of Witwatersrand, South Africa, and Hon. Dr Kailash Jagutpal, Minister of Health and Wellness, Government of Mauritius. In addition, Dr. Mory Keita answered questions about the latest Ebola Virus Disease (EVD) in the Democratic Republic of the Congo (DRC).
Concerns about COVID-19 featured in this immunization briefing for several reasons. First was the low coverage of COVID vaccines on the continent. Second was the way that COVID put demands on health workers’ time as well as on precautions to be undertaken, which limited the reach and coverage of immunization services for other vaccine preventable diseases (VPDs). Also, the resulting reduction in immunization coverage was responsible for other deadly outbreaks, notably measles. Between January and March 2022, for example, there was a 400% increase in measles cases compared to the same period last year.
 Dr. Impouma that COVID ‘taught the lesson’ that catch-up campaigns for VPDs were not only necessary but could be handled successfully. Finally, health services learned the importance of integration, whether joining COVID and Yellow Fever vaccination efforts in Ghana or integrating COVID with maternal and child services and immunizations. Ultimately, health workers learned that by strengthening ‘routine’ immunization, health systems overall could be strengthened thus, making progress on achieving Health For all through Universal Health Coverage.
Dr. Impouma that COVID ‘taught the lesson’ that catch-up campaigns for VPDs were not only necessary but could be handled successfully. Finally, health services learned the importance of integration, whether joining COVID and Yellow Fever vaccination efforts in Ghana or integrating COVID with maternal and child services and immunizations. Ultimately, health workers learned that by strengthening ‘routine’ immunization, health systems overall could be strengthened thus, making progress on achieving Health For all through Universal Health Coverage.
Dr. Jagutpal shared key considerations for successful life-course immunization programs. Mauritius offers free, universal vaccination from birth. Thirty VPDs are addressed ranging from Human Papilloma Virus to flu and not of course, COVID-19. Success is based on involvement of all stakeholders through regular meetings where real time decisions can be made. Mauritius in one of the first to formalize the COVID Vaccine Pass Card and has achieved 60% full vaccine coverage including booster shots.
Prof Rees noted that the term ‘routine services’ makes vaccines seem boring and less important, when in fact, they should be seen as “Core Services”. This central role of vaccines goes beyond preventing specific diseases. By saving children’s lives and reducing the time demands on parents who care for children suffering VPDs, immunization promotes human development, reduces poverty, enhances the economy, and strengthens employment. There remain children who have had no vaccines. Identifying these ‘zero dose’ children and the communities in which they cluster can help us focus on ameliorating the vulnerabilities of their families and bring multi-sectoral resources to bear on strengthening poor communities.
Dr Keita reviewed the two recent cases, now deaths from Ebola in Équateur Province in DRC, its third EVD outbreak. Ebola vaccine teams have started working, reaching 78 contacts. He lamented that much of the DRC has a natural ecological predisposition for the animal reservoirs of Ebola, so more effort on making regular vaccines and treatment available is required. As Prof Rees pointed out, this setting is a perfect example of the need for a One Health approach to many of our health challenges which are zoonotic in nature. Even with coronaviruses, animal reservoirs are a central element of transmission.
Additional research is recommended in several areas. The slowly increasing laboratory capacity in Africa was mentioned. It contributed to finding Omicron and its variants. Potential new ones may have been identified recently. Seropositivity analysis has found that 80-90% of people tested may already have COVID antibodies. Research can clarify the role of vaccines in these circumstances. Research as well as regular program monitoring is still needed to determine the factors that may cause children to miss vaccines. It is often not the case that parents are ‘hesitant’, but that system and community factors combine to prevent them from seeking care. Research can also assist in finding vaccines and tools for tackling other deadly pathogens such as Lassa Fever.
Vaccines save lives from endemic diseases, but in the long-term vaccinated families and communities can fight poverty which itself is a leading factor in illness and death. This will accomplish the theme of this year’s observance, “Long Life for All.”
Advocacy &Vaccine Bill Brieger | 25 Apr 2022
World Immunization Week Starts with World Malaria Day
 One might think initially that the convergence of World Malaria Day and World Immunization Week would simply be a coincidence. This year there is a major connection since WHO has approved the first ever RTS,S/AS01 malaria vaccine which has undergone decades to clinical testing and most recently, a successful 3-year pilot intervention in Malawi, Kenya, and Ghana.
One might think initially that the convergence of World Malaria Day and World Immunization Week would simply be a coincidence. This year there is a major connection since WHO has approved the first ever RTS,S/AS01 malaria vaccine which has undergone decades to clinical testing and most recently, a successful 3-year pilot intervention in Malawi, Kenya, and Ghana.
 During her keynote address at the Johns Hopkins Malaria Institute’s World Malaria Day Webinar today, The WHO Regional Director for the African Region, Dr. Matshidiso Moeti, stressed the importance of integrated disease control efforts drawing on the region’s efforts to tackle neglected tropical diseases, COVID-19 and of course, malaria. She highlighted the importance of surveillance, and in That context pointed out a serious fact. The population of sub-Saharan Africa had doubled since the start of the Roll Back Malaria initiative, meaning that to achieve the same level of coverage of key interventions, one needs to reach many more people, whether for malaria control or child immunization.
During her keynote address at the Johns Hopkins Malaria Institute’s World Malaria Day Webinar today, The WHO Regional Director for the African Region, Dr. Matshidiso Moeti, stressed the importance of integrated disease control efforts drawing on the region’s efforts to tackle neglected tropical diseases, COVID-19 and of course, malaria. She highlighted the importance of surveillance, and in That context pointed out a serious fact. The population of sub-Saharan Africa had doubled since the start of the Roll Back Malaria initiative, meaning that to achieve the same level of coverage of key interventions, one needs to reach many more people, whether for malaria control or child immunization.
Thus, increasing targets and goals affect both immunization and malaria programs, as well as efforts to roll out the malaria vaccine. At present there is only one producer of the vaccine, GlaxoSmithKline, and while that company is working with another company in India to produce RTS,S in the global south, GSK is maintaining control of the AS01 adjuvant. Production targets have so far been geared to meeting the needs in the pilot districts of the three intervention countries, and for the foreseeable future this will address less than 10% of need in P. falciparum endemic areas, especially in Africa.
 WHO and partners including UNICEF and GAVI are in the process of figuring out equitable ways to distribute what is available now and encouraging the ramp up of vaccine production. The need to vaccine technology transfer to Africa is also being considered. Additionally, eyes are focused on new malaria vaccine candidates which might come on board in about five years.
WHO and partners including UNICEF and GAVI are in the process of figuring out equitable ways to distribute what is available now and encouraging the ramp up of vaccine production. The need to vaccine technology transfer to Africa is also being considered. Additionally, eyes are focused on new malaria vaccine candidates which might come on board in about five years.
The current malaria vaccine, while reducing severe disease, does not have the highest efficacy, and experts caution that is is therefore, not a silver bullet. They do explain that the vaccine is an important addition to the malaria toolkit, and should be a central part of integrated malaria control planning. At present though, we are not only running in place to meet the needs of an ever increasing number of children at risk, and we also must cope in an ethical and efficient way with limited supplies of the vaccine for the near future. This is the double challenge to start Malaria Day and Vaccine Week.
Vaccine Bill Brieger | 07 Oct 2021
The RTS,S Malaria Vaccine: Logistics Are the Next Issue
The World Health Organization and its Global Malaria Program are happily announcing approval of the RTS,S/AS01 (RTS,S) malaria vaccine after many years of testing. Though research on this particular vaccine stretches back to the 1980s, the most recent test has been a pilot program in Ghana, Kenya and Malawi that has reached more than 800,000 children since 2019 in real life district health settings. Because the vaccine is not 100% effective, WHO Director-General Dr Tedros Adhanom Ghebreyesus notes that the intervention will compliment other efforts such that by “Using this vaccine on top of existing tools to prevent malaria could save tens of thousands of young lives each year.”
 Specifically, WHO explains that he RTS,S/AS01 malaria vaccine would be used “for the prevention of P. falciparum malaria in children living in regions with moderate to high transmission as defined by WHO.” RTS,S/AS01 malaria vaccine requires a “schedule of 4 doses in children from 5 months of age for the reduction of malaria disease and burden.”
Specifically, WHO explains that he RTS,S/AS01 malaria vaccine would be used “for the prevention of P. falciparum malaria in children living in regions with moderate to high transmission as defined by WHO.” RTS,S/AS01 malaria vaccine requires a “schedule of 4 doses in children from 5 months of age for the reduction of malaria disease and burden.”
The vaccine was found to have a strong safety profile, and in keeping with the concept of using it together with other preventive measures it produces, “Significant reduction (30%) in deadly severe malaria, even when introduced in areas where insecticide-treated nets are widely used and there is good access to diagnosis and treatment.”
The pilot effort was supported at the global and country levels by WHO, PATH, UNICEF and GlaxoSmithKline (GSK) in collaboration with the health systems of the three countries. An important component of the pilot effort was learning about delivery process, which in this case meant collaboration with district health services including overall childhood immunization programs. In fact, because of the link with vaccinations, children who were not reached with other malaria services had a better chance of getting protection from the vaccine.
It is important to state that WHO approval of RTS,S does not mean that malaria vaccine research has been complete. Several other vaccine candidates are currently in the research pipeline. In addition, the current COVID-19 vaccine efforts have led researchers to consider different approaches to malaria vaccine development.
Approval by WHO is just the beginning of the logistical and policy challenge up and down the supply chain. First, there are questions of production capacity. Secondly, Funding must be secured such as the assistance that Gavi (the Vaccine Alliance), GFATM (the Global Fund to Fight AIDS, Tuberculosis and Malaria), and Unitaid have provided to low- and middle-income countries to promote their immunization and health programs. In August Gavi announced that, “Gavi, MedAccess and GlaxoSmithKline (GSK) will join forces to guarantee continued production of the RTS,S antigen for the RTS,S/AS01e malaria vaccine
A third issue is obtaining regulatory approval in malaria endemic countries that wish to use the vaccine. Fourth, lessons on management of the vaccine delivery within both malaria and child health services on the ground, including community involvement, need to be shared with other countries in the region.
More than 30 years into the development and application of the RTS,S malaria vaccine, we are in a way just getting started when it comes to figuring out how to reach children and save their lives.
Elimination &Vaccine Bill Brieger | 23 Aug 2021
Malaria Vaccine Approval Nearing
Over the coming three days the Malaria Vaccine Implementation Programme (MVIP) Advisory Group in its capacity as SAGE/MPAG Working Group will conduct a full evidence review of the RTS,S/AS01 malaria vaccine and develop proposed recommendations for Strategic Advisory Group of Experts (SAGE) on Immunization and MPAG. This comes on the heels of the recent 74th World Health Assembly Resolution that, “Urges Member States to step up the pace of progress through plans and approaches that are consistent with WHO’s updated global malaria strategy and the WHO Guidelines for malaria. It calls on countries to extend investment in and support for health services, ensuring no one is left behind; sustain and scale up sufficient funding for the global malaria response; and boost investment in the research and development of new tools.”
 The large scale pilot intervention of the RTS,S/AS01 malaria vaccine started two years ago in selected districts in three countries countries: Ghana, Kenya and Malawi. For example, “Two years on from the launch of a pilot programme, more than 1.7 million doses of the world’s first malaria vaccine have been administered in Ghana, benefitting more than 650,000 children with additional malaria protection.” WHO says that, “Insights generated by the pilot implementation will inform a WHO recommendation on broader use of the vaccine across sub-Saharan Africa,” which will then be considered by global advisory bodies for immunization and malaria, i.e. the SAGE and MPAG.
The large scale pilot intervention of the RTS,S/AS01 malaria vaccine started two years ago in selected districts in three countries countries: Ghana, Kenya and Malawi. For example, “Two years on from the launch of a pilot programme, more than 1.7 million doses of the world’s first malaria vaccine have been administered in Ghana, benefitting more than 650,000 children with additional malaria protection.” WHO says that, “Insights generated by the pilot implementation will inform a WHO recommendation on broader use of the vaccine across sub-Saharan Africa,” which will then be considered by global advisory bodies for immunization and malaria, i.e. the SAGE and MPAG.
WHO is asking the Working Group to address the following question, “Does the additional evidence on the feasibility, safety and impact of the RTS,S/AS01 vaccine support a WHO recommendation for use of the vaccine in children in sub-Saharan Africa beyond the current pilot implementation?” WHO has set the following meeting objectives:
- To examine and provide input to the Grading of Recommendations Assessment, Development and Evaluation (GRADE) evidence profiles of the quality of the evidence used to inform the recommendations;
- To review and interpret the evidence, with explicit consideration of the overall balance of benefits and harms;
- To formulate recommendations – in alignment with the endorsed 2019 RTS,S Framework for Decision – taking into account benefits, harms, values and preferences, feasibility, equity, acceptability, resource requirements and other factors, as appropriate.
Hopefully decisions will be forthcoming soon so that planning can get underway to address immunization as part of the overall malaria elimination effort.
Funding &Vaccine Bill Brieger | 04 Aug 2021
GAVI Press Release: Financing for Malaria Vaccine
Geneva/London, 4 August 2021 – Gavi, the Vaccine Alliance, GlaxoSmithKline (GSK) and MedAccess today announced an innovative financing agreement to guarantee continued production of the antigen for the RTS,S/AS01e malaria vaccine in advance of key decisions regarding its roll-out.
 The RTS,S/AS01e vaccine – the first malaria vaccine to be proven safe and effective in a large Phase 3 clinical trial – is currently being piloted in routine immunisation programmes in Ghana, Kenya and Malawi, through the Malaria Vaccine Implementation Programme (MVIP). The World Health Organization (WHO) is expected to decide later this year whether to recommend the vaccine for broader use based on data emerging from the MVIP. The Gavi Board will then decide whether to finance a new malaria vaccination programme for countries in sub-Saharan Africa. Following its investment of around US$ 700 million in the development of RTS,S,GSK has donated up to 10 million doses for the ongoing pilot programme.
The RTS,S/AS01e vaccine – the first malaria vaccine to be proven safe and effective in a large Phase 3 clinical trial – is currently being piloted in routine immunisation programmes in Ghana, Kenya and Malawi, through the Malaria Vaccine Implementation Programme (MVIP). The World Health Organization (WHO) is expected to decide later this year whether to recommend the vaccine for broader use based on data emerging from the MVIP. The Gavi Board will then decide whether to finance a new malaria vaccination programme for countries in sub-Saharan Africa. Following its investment of around US$ 700 million in the development of RTS,S,GSK has donated up to 10 million doses for the ongoing pilot programme.
In advance of the key decisions from WHO and Gavi and to address the associated uncertainty around future demand, Gavi, GSK and MedAccess have developed an innovative financing solution to ensure continued manufacturing of the vaccine antigen so that it will be immediately available should there be a positive decision to move forward.
Gavi will fund GSK’s continued manufacturing of the RTS,S antigen for a period of up to three years. If the Gavi Board decides to approve a malaria vaccination programme (following a positive WHO recommendation), GSK will credit the value of the Gavi-funded costs towards procurement of finished doses for the Gavi-supported programme. If the Gavi Board decides not to open a funding window for a malaria vaccination programme, MedAccess will replenish Gavi for the majority of costs incurred to that point.
This arrangement will ensure that vaccine doses made from the production of Gavi-funded bulk antigen can be supplied rapidly after a potential WHO vaccine recommendation and Gavi financing decisions. This will help accelerate vaccine access, if a programme is approved, by avoiding the long production ramp-up phase that would occur if GSK had to restart the dedicated antigen production facility.
A MedAccess analysis estimates that this continuous manufacture agreement could catalyse the vaccine reaching up to 7.5 million more children than would otherwise have been possible if there was a production delay.
“Malaria kills over a quarter of a million children every year; this vaccine has the potential to have a real impact on this toll,” said Dr Seth Berkley, CEO of Gavi, the Vaccine Alliance. “That’s why it is vital that we keep production lines running while waiting for important decisions around its use in African populations. This is innovative financing at its best: tackling risk and uncertainty to ensure access to what could be an important additional tool in the battle against malaria.”
“In 2020 we saw that risk-taking finance can accelerate the journey of new vaccines to market,” said Michael Anderson, CEO of MedAccess. “The same idea is at work in this agreement, where smart finance can unlock and secure access to an important product at faster pace. This unique partnership is a prime example of how science, public health expertise and innovative finance can combine to save lives.”
Thomas Breuer, Chief Global Health Officer, GSK, said: “Reaching an agreement to support continuous production of RTS,S bulk antigen is a significant achievement built on a unique funding solution and I congratulate all of the partners involved. Continuity of RTS,S manufacturing now will be crucial in how quickly we can offer malaria protection once WHO, Gavi and implementing countries agree to scale up demand.”
Separate to this agreement, GSK and Bharat Biotech of India will continue activities related to the antigen tech transfer to Bharat Biotech, which will become the sole supplier of the vaccine in 2029, an agreement announced by GSK, Bharat, and PATH earlier this year. GSK will ensure the continuous production of the adjuvant (AS01e).
A Phase 3 trial conducted over 5 years from 2009 to 2014 found that among children aged 5–17 months who received four doses of RTS,S/AS01e, the vaccine prevented approximately 4 in 10 (39%) cases of malaria over 4 years of follow-up and about 3 in 10 (29%) cases of severe malaria, with significant reductions also seen in overall hospital admissions as well as in admissions due to malaria or severe anaemia. The vaccine also reduced the need for blood transfusions, which are required to treat life-threatening malaria anaemia, by 29%.
RTS,S/AS01e is currently being piloted in three African countries (Ghana, Kenya, Malawi) and, despite COVID-19, has achieved and maintained high coverage levels. As of July 2021, two years after the start of vaccinations, more than 2 million RTS,S/AS01e doses have been administered across the three countries and more than 740,000 children have been reached with at least one dose of vaccine.
Ministries of Health are leading the implementation of the vaccine, which is being delivered through routine immunisation programmes, with WHO playing a coordinating role, working in collaboration with GSK, PATH, Unicef and a range of other partners. The programme is funded by Gavi, the Global Fund and Unitaid, with doses donated by GSK, and was designed to address several outstanding questions related to the public health use of the vaccine following the Phase 3 trial.
COVID-19 &Drug Development &Elimination &Funding &Plasmodium/Parasite &Resistance &Vaccine Bill Brieger | 17 Sep 2020
Malaria News Today 2020-09-17
 Leading off our news update are findings from eastern Kenya about a genetic blood grouping that may help prevent malaria. While government leaders in the Asia-Pacific region committed to eliminating malaria, a report from the Gates Foundation explains how COVID-19 has set progress back and without new tools it may take more than 25 years to rid the world of the disease. In that light, Novartis is staking its finances on being able to make medicines that will be accessible and fight malaria. More details and the Gates video can be seen by clicking the links below.
Leading off our news update are findings from eastern Kenya about a genetic blood grouping that may help prevent malaria. While government leaders in the Asia-Pacific region committed to eliminating malaria, a report from the Gates Foundation explains how COVID-19 has set progress back and without new tools it may take more than 25 years to rid the world of the disease. In that light, Novartis is staking its finances on being able to make medicines that will be accessible and fight malaria. More details and the Gates video can be seen by clicking the links below.
How Dantu Blood Group protects against malaria
The secret of how the Dantu genetic blood variant helps to protect against malaria has been revealed for the first time by scientists at the Wellcome Sanger Institute, the University of Cambridge and the KEMRI-Wellcome Trust Research Programme, Kenya. The team found that red blood cells in people with the rare Dantu blood variant have a higher surface tension that prevents them from being invaded by the world’s deadliest malaria parasite, Plasmodium falciparum. The findings were published in Nature and could be significant in the wider battle against malaria.
In 2017, researchers discovered that the rare Dantu blood variant, which is found regularly only in parts of East Africa, provides some degree of protection against severe malaria. The intention behind this new study was to explain why. Red blood cell samples were collected from 42 healthy children in Kilifi, Kenya, who had either one, two or zero copies of the Dantu gene. The Dantu variant created cells with a higher surface tension—like a drum with a tighter skin. At a certain tension, malaria parasites were no longer able to enter the cell.
Novartis ties bond sale to malaria treatment access in sustainability push
Novartis raised 1.85 billion euros on Wednesday from the sale of a bond on which interest payments will rise if the drugmaker fails to expand access to medicines and programmes to combat malaria and leprosy in a number of developing countries.
Investors are increasingly pushing companies to improve their track record on environmental, social and governance (ESG) issues while sustainable investing grows in popularity, spurring an increase in sustainable debt issuance year after year. Novartis’ bond is only the third issue to date to link payments to creditors to company-wide sustainable development targets. By Yoruk Bahceli
Commitment to make Asia Pacific a malaria free region
Government officials from across Asia Pacific have come together during virtual Malaria Week 2020, to reaffirm their commitment to eliminating malaria and strengthening health systems to keep the region safe from health threats. Embracing the theme of “Inclusion. Integration. Innovation.”, officials called for increased collaboration and action to accelerate towards the goal of ending malaria in the region by 2030, at a time when major gains and regional progress are under threat due to disruptions caused by Covid-19.
It could take up to 25 years to eradicate malaria from Africa – Bill Gates
Bill Gates said: “Moving to malaria which is a very awful disease not just to the kids it kills but many kids whose brains are permanently damaged, the economic effects you have with malaria. If we don’t have new tools like vaccines or new ways of killing mosquitoes, it would probably take more than 25 years to get rid of malaria. If we get the new tools and they work, we think it can be done in under 20 years. So the malaria field is both trying to keep the number of deaths down, and we have to deal with the resistance that comes up, that the mosquitoes develop.”
Gates Foundation Report notes that, “We’ve been set back about 25 years in about 25 weeks.” Extreme poverty increased 7% because of COVID-19. In a video included in the Foundation’s report, Bill Gates explains how COVID-19 disrupts the fight against malaria.