Economics &ITNs &Mosquitoes &Vector Control Bill Brieger | 25 Oct 2017
Mis-Use of Insecticide Treated Nets May Actually Be Rational
People have sometimes question whether insecticide treated nets (ITNs) provided for free are valued by the recipients. Although this is not usually a specific question in surveys, researchers found in a review of 14 national household surveys that free nets received through a campaign were six times more likely to be given away than nets obtained through other avenues such as routine health care or purchased from shops.
 Giving nets away to other potential users, not hanging nets or not sleeping under nets at least imply that the nets could potentially be used for their intended purpose. What concerns many is that nets may be used for unintended and inappropriate reasons. Often the evidence is anecdotal, but photos from Nigeria and Burkina Faso shown here document cases where nets were found to cover kiosks, make football goalposts, protect vegetable seedlings and fence in livestock.
Giving nets away to other potential users, not hanging nets or not sleeping under nets at least imply that the nets could potentially be used for their intended purpose. What concerns many is that nets may be used for unintended and inappropriate reasons. Often the evidence is anecdotal, but photos from Nigeria and Burkina Faso shown here document cases where nets were found to cover kiosks, make football goalposts, protect vegetable seedlings and fence in livestock.
Newspapers tend to quote horrified health or academic staff when reporting this, such as this statement from Mozambique, “The nets go straight out of the bag into the sea.” The Times said that net misuse squandered money and lives when they observed that “Malaria nets distributed by the Global Fund have ended up being used for fishing, protecting livestock and to make wedding dresses.”
 Two years ago the New York Times reported that, “Across Africa, from the mud flats of Nigeria to the coral reefs off Mozambique, mosquito-net fishing is a growing problem, an unintended consequence of one of the biggest and most celebrated public health campaigns in recent years.”5 Not only were people not being protected from malaria, but the pesticide in these ‘fishing nets’ was causing environmental damage. The article explains that the problem of such misuse may be small, but that survey respondents are very unlikely to admit to alternative uses to interviewers.
Two years ago the New York Times reported that, “Across Africa, from the mud flats of Nigeria to the coral reefs off Mozambique, mosquito-net fishing is a growing problem, an unintended consequence of one of the biggest and most celebrated public health campaigns in recent years.”5 Not only were people not being protected from malaria, but the pesticide in these ‘fishing nets’ was causing environmental damage. The article explains that the problem of such misuse may be small, but that survey respondents are very unlikely to admit to alternative uses to interviewers.
Similarly El Pais website featured an article on malaria in Angola this year with a striking lead photo of children fishing in the marshes near their village in Cubal with a LLIN. A video from the New York Times frames this problem in a stark choice: sleep under the nets to prevent malaria or them it to catch fish and prevent starvation.[v]
 More recently, researchers who examined net use data from Kenya and Vanuatu found that alternative LLIN use is likely to emerge in impoverished populations where these practices had economic benefits like alternative ITN uses sewing bednets together to create larger fishing nets, drying fish on nets spread along the beach, seedling crop protection, and granary protection. The authors raise the question whether such uses are in fact rational from the perspective of poor people.
More recently, researchers who examined net use data from Kenya and Vanuatu found that alternative LLIN use is likely to emerge in impoverished populations where these practices had economic benefits like alternative ITN uses sewing bednets together to create larger fishing nets, drying fish on nets spread along the beach, seedling crop protection, and granary protection. The authors raise the question whether such uses are in fact rational from the perspective of poor people.
An important fact is that not all ovserved ‘mis-use’ of nets is really inappropriate use. A qualitative study in the Kilifi area of coastal Kenya demonstrated local ‘recycling’ of old ineffective nets. The researchers clearly found that in rural, peri-urban and urban settings people adopted innovative and beneficial ways of re-using old, expired nets, and those that were damaged beyond repair. Fencing for livestock, seedlings and crops were the most common uses in this predominantly agricultural area. Other domestic uses were well/water container covers, window screens, and braiding into rope that could be used for making chairs, beds and clotheslines. Recreational uses such as making footballs, football goals and children’s swings were reported
What we have learned here is that we should not jump to conclusions when we observe a LLIN that is set up for another purpose than protecting people from mosquito bites. Alternative uses of newly acquired nets do occur and may seem economically rational to poor communities. At the same time we must ensure that mass campaigns pay more attention to community involvement, culturally appropriate health education and onsite follow-up, especially the involvement of community health workers. Until such time as feasible safe disposal of ‘retired’ nets can be established, it would be good to work with communities to help them repurpose those nets that no longer can protect people from malaria.
Case Management &Resistance Bill Brieger | 22 Oct 2017
The Need to Prevent the Spread of Malaria Drug Resistance to Africa
Chike Nwangwu is a Monitoring and Evaluation Specialist who is currently working on his Doctor of Public Health (DrPH) degree at the Johns Hopkins Bloomberg School of Public Health. Here he presents an overview of the threat of parasite resistance to first-line antimalarial drugs and the need to prevent the spread of this problem in Africa which beard the greatest burden of the global malaria problem.
Malaria, remains one of the most pervasive and most malicious parasitic infections worldwide. Malaria is caused by Plasmodium parasites when they enter the human body. There are currently five known plasmodium species that cause malaria in humans- P. falciparum and P. vivax are the most prevalent globally. These parasites are transmitted through the bites of infected female anopheles mosquitoes “malaria-vectors” which perpetuate the spread of the parasite from human-human or from host- human.
Globally, according to the WHO, an estimated 212 million cases of malaria and 429 000 malaria related deaths occurred in 2015.[1] The global share of malaria is spread disproportionately across regions; Over 90% of global malaria cases and deaths occurred in the African region, with over 70% of the global burden in one sub region-Sub Saharan Africa. In areas with high transmission of malaria, children under 5 are at the highest risk to infection and death; more than two thirds of all malaria deaths occur in this age group.[2]
 Although malaria remains a global concern, malaria is preventable and curable. Increased efforts in malaria prevention and treatment within the past two decades has led to revolutionary success- 6.8 million lives have been saved globally and malaria mortality cut by 45% since 2001.[3] Globally, within a five-year interval (2010-2015) new malaria transmission and mortality in children under 5 years of age fell by 21% and 29% respectively. This has been the one the greatest public health successes in recent years [4]
Although malaria remains a global concern, malaria is preventable and curable. Increased efforts in malaria prevention and treatment within the past two decades has led to revolutionary success- 6.8 million lives have been saved globally and malaria mortality cut by 45% since 2001.[3] Globally, within a five-year interval (2010-2015) new malaria transmission and mortality in children under 5 years of age fell by 21% and 29% respectively. This has been the one the greatest public health successes in recent years [4]
The improvement of malaria indices aligns with intensification of efforts, through funding, research, innovation pushing the scale up of key malaria interventions in the malaria prevention- diagnostic- treatment cascade. For example, in Sub-Saharan Africa where malaria is most prevalent, there has been a recorded 48% increment in Insecticide Treated Net (ITN) usage since 2005, 15% rise in chemoprevention in pregnant women and within the same time frame diagnostic testing increased from 40% of suspected malaria cases to 76%.[5]
Treatment/ Emergence of insecticide and drug resistance
Malaria treatment plays a key role in controlling its transmission. First, prompt and effective treatment of malaria prevents progression to severe disease and limits the development of gametocytes, thus blocking transmission of parasites from humans to mosquitoes.[6] Drugs can also be used to prevent malaria in endemic populations, including various strategies of chemoprophylaxis, intermittent preventive therapy, and mass drug administration can be effective.[7] Like other interventions, availability and use of antimalarial has been a success. However, this has also come with some challenges. The emergence of resistance, particularly in P. falciparum and P. vivax to antimalarial-quinine and sulfadoxine-pyrimethamine, has been a major contributor to reported resurgences of malaria in the last three decades.[8]
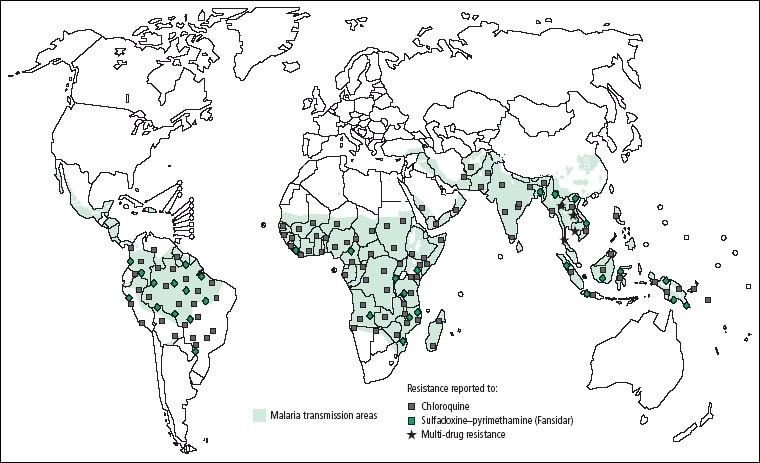
Distribution of reported resistance to antimalarials. As at 2005, antimalarial resistance was is established in 81 of the 92 countries where the disease was endemic (WHO, 2004)
Falciparum resistance first developed in some areas in Southeast Asia, Oceania, and South America before the 70’s eventually the parasite became resistant to other drugs (sulfadoxine/ pyrimethamine, mefloquine, halofantrine, and quinine. Drug-resistant P. vivax was first identified in 1989 in one region and later spread to other regions of the world.[9] As at 2005, antimalaria resistance to chloroquine and sulfadoxine-pyrimethamine was established in 81 of the 92 countries where the disease was endemic. (Figure 1) In 2005, alongside acetaminophen, antimalarial were among the most commonly abused medications in the African region, with the majority of the population having detectable amounts of chloroquine in the blood.[10]
Antimalarial drug resistance is the decrease in viability of an antimalarial to cure an infection. Parasite resistance results in a delayed or partial clearance of parasites from the blood when a person is being treated with an antimalarial.[11] Antimalaria resistance occurs as the byproduct of at least one mutation in the genome of the parasite, giving an advantageous capacity to evade the impacts of the drug. Within the human host, drug resistance develops gradually. First, a modest number of drug-resistant parasites survive exposure to the drug whilst the drug-sensitive parasites are eliminated. In the absence of additional drugs and competition from drug-sensitive pathogens, the drug-resistant parasites proliferate and their populace develops. This new population is therefore resistant to additional malaria medications of the same type.
Following the discovery of resistance to quinine and sulfadoxine-pyrimethamine, the development of resistance was initially forestalled by the utilization of a new class of malaria drugs – Artemisinin-derivative combinations. These ACTs (Artemisinin Combination Therapy) work by combining artemisinin and an active partner drug with different mechanisms of action. The WHO, with guidance from extensive drug efficacy tests and research, recommends the use of 5 types of ACTs for treatment of uncomplicated malaria caused by the P. falciparum parasite. By 2014, ACTs have been adopted as first-line treatment policy in 81 countries.[12]
Although ACT use has been a breakthrough in malaria treatment, development of resistance to de novo ACTs poses one of the greatest threats to malaria control efforts. P. falciparum resistance to artemisinin has been detected in five countries of the Greater Mekong sub-region (Lao, Myanmar, Thailand, Cambodia, and Vietnam). To date P. vivax resistance to an ACT has not been detected.
Artemisinin resistance is currently defined within the confines of delayed parasite clearance; it represents partial/relative resistance-i.e. most patients who have delayed parasite clearance do not necessarily have treatment failure. Following treatment with an ACT, infections are still cleared, as long as the partner drug remains effective. Various factors are believed to contribute to the development and spread of resistance to artemisinin; use of oral artesunate monotherapies (oAMT) inclusive.
 A global response has been mounted to curtail the spread of ACT resistance to other regions, especially to regions like Sub-Saharan Africa. Research on the mechanisms of drug resistance has steered efforts in the direction, recently the identification of the PfKelch13 (K13) mutations has allowed for a more refined definition of artemisinin resistance that includes information on the genotype. [13] In addition, stricter policies have been developed for malaria control; Therapeutic efficacy studies (TES) are conducted and used as the main reference from which national malaria control programmes determine their national treatment policy.[14] These studies help to ensure the efficacy of treatments with recommendations to ensure that these medicines are monitored through surveillance at least once every 24 months at established sentinel sites and in regions with emerging resistance, the creation of additional sentinel surveillance sites. [15]
A global response has been mounted to curtail the spread of ACT resistance to other regions, especially to regions like Sub-Saharan Africa. Research on the mechanisms of drug resistance has steered efforts in the direction, recently the identification of the PfKelch13 (K13) mutations has allowed for a more refined definition of artemisinin resistance that includes information on the genotype. [13] In addition, stricter policies have been developed for malaria control; Therapeutic efficacy studies (TES) are conducted and used as the main reference from which national malaria control programmes determine their national treatment policy.[14] These studies help to ensure the efficacy of treatments with recommendations to ensure that these medicines are monitored through surveillance at least once every 24 months at established sentinel sites and in regions with emerging resistance, the creation of additional sentinel surveillance sites. [15]
Preventing and containing antimalarial drug resistance- Recommendations to countries
As research is being done to fully understand the mechanisms of antimalarial resistance; basic recommendations to limit its spread have been disseminated.[16] First, the production and use of oral artemisinin-based monotherapy should be halted and access to the use of quality-assured ACTs for the treatment of falciparum malaria should be ensured. In countries where antimalarial treatments remain fully efficacious; correct medicine use must be promoted, with weight placed on encouraging diagnostic testing, quality-assured treatment, and good patient adherence to the treatment. Lastly, to reduce the burden of the disease, and prevent the spread of resistance, in regions where there is still high transmission, intensification of malaria control efforts is key, rapid elimination of falciparum malaria would accelerate efforts.
- [1] World Malaria Report 2016, World Health Organization, Geneva, 2016
- [2] ibid
- [3] CDC, Malaria Fast Facts 2017
- [4] ibid
- [5] World Malaria Report, 2016
- [6] Gosling RD, Okell L, Mosha J, Chandramohan D. The role of antimalarial treatment in the elimination of malaria. Clin Microbiol Infect. 2011;17:1617–1623.
- [7] Greenwood B. Anti-malarial drugs and the prevention of malaria in the population of malaria endemic areas. Malar J. 2010;9
- [8] White NJ. Antimalarial drug resistance. J Clin Invest. 2004;113:1084–1092
- [9] CDC, Malaria Fast Facts, 2017
- [10] White NJ. Antimalarial drug resistance. J Clin Invest. 2004;113:1084–1092.
- [11] Peter B. Bloland, Drug resistance in malaria, World Health Organization, 2001
- [12] World Malaria Report, 2016, World Health Organization, Geneva,2016
- [13] Artemisinin and artemisinin-based combination therapy resistance April 2017,World Health Organization, 2017
- [14] Responding to antimalarial drug resistance, World Health Organization, 2017: http://www.who.int/malaria/areas/drug_resistance/overview/en/
- [15] ibid
- [16] Ibid
Community &IPTp &Malaria in Pregnancy Bill Brieger | 21 Oct 2017
Committing to Preventing Malaria in Pregnancy From the National to State to Local Level in Nigeria
Bright Orji recently shared an overview of the Transforming Intermittent Preventive Treatment for Optimal Pregnancy (TIPTOP) Project in Nigeria, a joint venture to protect pregnant women from malaria organized by Jhpiego with support from Unitaid, the National Malaria Elimination Program, The State Ministries of Health in Ebonyi, Niger and Ondo and the local communities. He shares some highlights from the project launch this past week. The project will strengthening antenatal care services to reach out and involve communities in the grassroots delivery of intermittent preventive treatment of malaria in pregnancy (IPTp).
Among those in attendance were wife of the Ebonyi State Executive Governor and representatives from the State Ministry of Health, the State Malaria Elimination Program, the State Primary Health Care Development Agency, the Ebonyi State House of Assembly, the Ministry of Justice, the Ministry of Local Government, the Ministry of Women Affairs, the School of Nursing and Midwifery, the School of Health Technology Ngbo, the Ohaukwu local government council and the community members.
The media documented the active participation, involvement and commitment by all stakeholders. Other partners present were the World Health Organization representing all UN Agencies in Nigeria and ISGlobal of Barcelona. Furthermore, the villages, families, and traditional rulers of the 16 communities that made up Ohaukwu Communitywelcomed the new project.

In order to emphasize an integrated approach to preventing malaria in pregnancy Ebonyi State, pregnant women given long lasting nets during the TIPTOP launch
Her Excellency Rachel Umahi, wife of the Ebonyi Governor said that, “TIPTOP project came at the right time, and I pledge to join hands to stop malaria in the state.” She was joined by the Ohaukwu Local Government Chairman Barr Clement Oda who shared that, “Today marks a special day in the history of Ohaukwu LGA, Ebonyi State and Nigeria at large as TIPTOP project launch will put the state and her people in the global map. This TIPTOP project will receive a very good support and cooperation from my administration. We shall not relent on what or things we need to do to make this project a success in Ohaukwu LGA worthy for this project.”
The National Coordinator National Malaria Elimination Program, Dr. Bala Audu, explained that, “The choice of Ebonyi state and Ohaukwu LGA in particular is not unconnected with the low utilization of the antenatal care services and low performance in IPTp utilization when compared with other LGAs in the southeastern region. We hope the LGA and the state will use this opportunity to redeem her image in malaria in pregnancy performance in Nigeria.” He pledged his support to Jhpiego and the malaria programs in the three participating states.
Dr. Ugo Okoli, Deputy Country Director Jhpiego in Nigeria pointed out the synergies possible within the state through noting that the, “Maternal and Child Survival Project funded by USAID will collaborate with TIPTOP in Ebonyi State to ensure that ANC is strengthened, and communities mobilized to utilize services.”
Bright Orji will provide updates from time to time in these efforts to reduce the high mortality through community efforts from malaria in pregnancy in Nigeria.
IPTp &Malaria in Pregnancy Bill Brieger | 18 Oct 2017
Transforming Intermittent Preventive Treatment For Optimal Pregnancy (TIPTOP) Project in Ebonyi State Nigeria
Bright Orji who is the Project Manager for the Jhpiego and UNITAID Transforming Intermittent Preventive Treatment For Optimal Pregnancy (TIPTOP) Project in Nigeria shares remarks that introduce the program in Ebonyi State of Nigeria.
The project will help protect pregnant women from malaria. Malaria is very dangerous to pregnant women and unborn babies. It causes abortion, low birth weight in babies as well as responsible for about 11% (6,050) of maternal deaths of Nigerian women

Jhpiego’s original community IPTp in Akwa Ibom State involved community volunteers in preventing malaria in pregnancy
Building on Jhpiego’s effort to ensure Intermittent preventive treatment in pregnancy (IPTp) reaches all women in the community. Between 2007 and 2010, Jhpiego collaborated with the National Malaria Elimination Program (NMEP), Reproductive Health division of the Federal Ministry of Health and provided technical assistance to the Ministry of Health in Akwa Ibom State to introduce a community directed approach with a focus on malaria in pregnancy with support from the ExxonMobil Foundation. That project reached over 35,000 pregnant women representing an increase in IPTp uptake by 35.3% going from 21.7% at baseline to 57.0% at the endline.
With support coming from Unitaid, Jhpiego and her partners will be implementing Transforming Intermittent Preventive Treatment for optimal pregnancy – shortened to TIPTOP project reach all pregnant women in Ohaukwu, Ebonyi State (South-East), Suleja in Niger State (North Central and Akure south in Ondo State (South West).
These States were selected on the basis of malaria prevalence rate; national commitment to generate evidence across the six geographical zones; given that similar project has been implemented in Akwa Ibom State representing South-South, and Sokoto state representing North West. Poor status of IPTp interventions in the selected Local government areas; and to further complement our on-going efforts with Maternal and Child Survival Project funded by the United States Agency for International Development (USAID/MCSP); Presidential Malaria Initiatives (PMI), Global Health Funds for Tuberclosis, HIV/AIDs and Malaria.
In this effort, we will work with the National Malaria Elimination Program (NMEP) that is charged with the responsibility of coordinating all malaria prevention and control activities in Nigeria; Reproductive Health Division of the Family health department, Federal Ministry of Health, State Ministries of Health, Local Governments authorities, communities development partners including World Health Organization (WHO); UNICEF, World Bank and other stakeholders (PMI/USAID, AFENTH etc).
To do this, TIPTOP project Nigeria will use a two-pronged approach that will increase the number of pregnant women in the three states who receive key malaria in pregnancy interventions by:
- Strengthening ANC services in health facilities, ensuring that a strong foundation for MIP services is in place; and
- Using community directed intervention approach where Community health workers,
Supervised by these strengthened ANC facilities, to initiate MIP interventions at the community level and refer women to the nearest ANC facility

Antenatal Clinics are the base for organizing training and community involvement in delivering Intermittent malaria Preventive Treatment in Pregnancy
Both parts of this approach will also strengthen local capacity in training, supervision, project implementation and evaluation by working with local civil society organizations that have strong ties to the community. As a component of this project, TIPTOP will seek a model for integrating MIP and other prevention services on the platform of ANC. TIPTOP project has planned for operations research that will provide some lessons and evidence and these include:
- Household surveys to gain understanding how pregnant women think, where they receive services if they are not coming to the health centers, and how we can prove services they receive
- Anthropological study – that would investigate community acceptability of community IPTp
- Sulfadoxine-pyrimethamine (SP) resistance monitoring study and
- Economic study – cost-benefit analysis
We are aware of the challenges ahead, Prof. ‘Dipo Otolorin the former Country Director for Jhpiego and now the Snr. Technical and Programmatic Advisor will always say, “a stick of broom cannot sweep the street, but when you have a bunch of sticks sweeping becomes delightful”. This is an African aphorism for team building.
So, from beginning of the grant application and subsequent development of the approved country operational plan (COP); we have engaged the key stakeholders that work on malaria in Nigeria. This is because we need the collaboration, coordination and cooperation of everyone. We will work together to mobilize all the communities in these three states, conduct community census that will guide us to estimate adequate number of SP doses; enter every kindred, family, household and home of pregnant women. We will identify all the pregnant women, refer them to attend ANC, as well as administer the life-saving medicines to the eligible ones both at facility and community levels. NO PREGNANT WOMAN SHOULD DIE OF MALARIA, BECAUSE IT IS PREVENTABLE, TREATABLE AND WE HAVE EVIDENCE-BASED INTERVENTIONS TO PROTECT THEM.
By the end of the project we would have achieved the goal of increasing the number of women who receive MIP services through strengthened ANC and community-level interventions. TIPTOP project expects additional outcomes from this initiative and these include:
- Generate evidence for WHO policy change
- set stage for scale up of community intermittent preventive treatment during pregnancy (IPTp)
- Increased demand for quality assured sulfadoxine–pyrimethamine (SP) for IPTp and
With this project no pregnant woman should die from malaria. So let us all join hands to stop malaria – and make Nigeria a Malaria free nation!!!

