Asymptomatic &Elimination &Eradication &Monkeys &Mosquitoes &Resistance &Vaccine Bill Brieger | 23 Aug 2019
Biology and Malaria Eradication: Are there Barriers?
During a press conference prior to the release of the executive summary of 3-year study of trends and future projections for the factors and determinants that underpin malaria by its Strategic Advisory Group on Malaria Eradication (SAGme), WHO outlined some hopeful signs emanating from the SAGme including
- Lack of biological barriers to malaria eradication
- Recognition of the massive social and economic benefits that would provide a return on investment in eradication, and
- Megatrends in the areas of factors such as land use, climate, migration, urbanization that could inhibit malaria transmission
 Concerning the first point, the executive summary notes that, “We did not identify biological or environmental barriers to malaria eradication. In addition, our review of models accounting for a variety of global trends in the human and biophysical environment over the next three decades suggest that the world of the future will have much less malaria to contend with.”
Concerning the first point, the executive summary notes that, “We did not identify biological or environmental barriers to malaria eradication. In addition, our review of models accounting for a variety of global trends in the human and biophysical environment over the next three decades suggest that the world of the future will have much less malaria to contend with.”
The group did agree that, “using current tools, we will still have 11 million cases of malaria in Africa in 2050.” So one wonders whether there are biological barriers or not.
Interestingly the group did identify, “Potential biological threats to malaria eradication include development of insecticide and antimalarial drug resistance, vector population dynamics and altered vector behaviour. For example, Anopheles vectors might adapt to breeding in polluted water, and mosquito vector species newly introduced to Africa, such as Anopheles stephensi, could spread more widely into urban settings.”
This discussion harkens back to an important conceptual article by Bruce Aylward and colleagues that raised the question in the American Journal of Public Health, “When Is a Disease Eradicable?” They outlined three important criteria that had been proposed at two international conferences in 1997 and 1998.
- biological and technical feasibility
- costs and benefits, and
- societal and political considerations
Their further expansion on the biological issues using smallpox as an example is instructive. They noted that not only are humans essential for the life cycle of the organism, but that there was no other reservoir for the causative virus, and the virus could not amplify in the environment. In short, there were no vectors, as in the case of malaria. The relatively recent documentation of transmission of malaria between humans and other primates of different plasmodium species is another biological concern. At this point, Malaysia, for example, is reporting more cases of Plasmodium knowlesi in humans that either P vivax or P falciparum.
Another biological issue identified by Aylward and colleagues was the fact that smallpox had one effective and proven intervention, the vaccine. Application of the vaccine could be targeted using photograph disease recognition cards as the signs were quite specific to the disease. Malaria has several effective interventions, but most strategies emphasize the importance of using a combination of these, and implementation is met with a number of management and logistical challenges. The signs and symptoms of malaria are confused with a number of febrile illnesses.
Finally, two other issues raised concern. Insecticide resistance was recognized in the first malaria eradication effort, and is raising its head again, as pointed out by SAGme. Comparing smallpox and yaws, the challenge of latent or sub-clinical/asymptomatic infection was mentioned. Malaria too, is beleaguered with this problem.
Clearly, we must not lose momentum in the marathon (not a race) to eliminate malaria, but we must, as WHO stressed at the press conference, increase our research and development efforts to strengthen existing tools and develop new once to address the biological and logistical challenges.
Conflict &Diagnosis &Ebola &ITNs &Mosquitoes &Plasmodium/Parasite &Resistance &Vaccine Bill Brieger | 29 Jul 2019
Tropical Health Update 2019-07-28: Ebola and Malaria Crises
This posting focuses on Malaria and Ebola, both of which have been the recent focus of some disturbing news. The malaria community has been disturbed by the clear documentation of resistance to drugs in Southeast Asia. Those working to contain Ebola in the northeast of the Democratic Republic of Congo saw a change in political leadership even in light of continued violence and potential cross-border spread.
Malaria Drug Resistance
Several sources reported on studies in the Lancet Infectious Diseases concerning the spread of Multidrug-Resistant Malaria in Southeast Asia. Reuters explained that by sing genomic surveillance, researchers concurred that “strains of malaria resistant to two key anti-malarial medicines are becoming more dominant” and “spread aggressively, replacing local malaria parasites,” becoming the dominant strains in Vietnam, Laos and northeastern Thailand.”
 The focus was on “the first-line treatment for malaria in many parts of Asia in the last decade has been a combination of dihydroartemisinin and piperaquine, also known as DHA-PPQ,” and resistance had begun to spread in Cambodia between 2007 and 2013. Authors of the study noted that while, “”Other drugs may be effective at the moment, but the situation is extremely fragile, and this study highlights that urgent action is needed.” They further warned of an 9impending Global Health Emergency.
The focus was on “the first-line treatment for malaria in many parts of Asia in the last decade has been a combination of dihydroartemisinin and piperaquine, also known as DHA-PPQ,” and resistance had begun to spread in Cambodia between 2007 and 2013. Authors of the study noted that while, “”Other drugs may be effective at the moment, but the situation is extremely fragile, and this study highlights that urgent action is needed.” They further warned of an 9impending Global Health Emergency.
NPR notes that “Malaria drugs are failing at an “alarming” rate in Southeast Asia” and provided some historical context about malaria drug resistance arising in this region since the middle of the 20th century. “Somehow antimalarial drug resistance always starts in that part of the world,” says Arjen Dondorp, who leads malaria research at the Mahidol Oxford Tropical Medicine Research Unit in Bangkok and who was a lead author of the report about the randomized trial. Ironically, “one reason could have something to do with the relatively low levels of malaria there. When resistant parasites emerge, they are not competing against a dominant nonresistant strain of malaria and are possibly able to spread easier.
When we are talking about monitoring resistance in low resource and logistically and politically challenging areas, we need to think of appropriate diagnostic tools at the molecular level. Researchers in Guinea-Bissau conducted a proof of concept study and used malaria rapid diagnostic tests applied for parallel sequencing for surveillance of molecular markers. While they noted that, “Factors such as RDT storage prior to DNA extraction and parasitaemia of the infection are likely to have an effect on whether or not parasite DNA can be successfully analysed … obtaining the necessary data from used RDTs, despite suboptimal output, becomes a feasible, affordable and hence a justifiable method.”
A Look at Insecticide Treated Nets
On a positive note, Voice of America provides more details on the insecticide treated net (ITN) monitoring tool developed called “SmartNet” by Dr Krezanoski in collaboration with the Consortium for Affordable Medical Technologies in Uganda. The net uses strips of conductive fabric to detect when it’s in use. Dr. Krezanoski was happy to find that people given the net used it no differently that if they were not being observed. The test nets made it clear who what using and not using this valuable health investment and when it was in use. Such fine tuning will be deployed to design interventions to educate net users based on their real-life use patterns.
Another important net issue is local beliefs that may influence use. We can find out when people use nets, but we also need to determine why. In Tanzania, researchers found that people think mosquitoes that bite in the early evening when people are outside relaxing are harmless. As one community member said, “I only fear those that bite after midnight. We’ve always been told that malaria is spread by mosquitoes that bite after midnight.”
Even if people do use their ITNs correctly, we still need to worry about insecticide resistance. A study in Afghanistan reported that, “Resistance to different groups of insecticides in the field populations of An. stephensi from Kunar, Laghman and Nangarhar Provinces of Afghanistan is caused by a range of metabolic and site insensitivity mechanisms.” The authors conclude that vector control programs need to be better prepared to implement insecticide resistance management strategies.
Ebola Crisis Becomes (More) Political
Headlines such as “Congo health minister resigns over response to Ebola crisis” confronted the global health community this week. this happened after the DRC’s relatively new president took control of the response. The President set up a new government office to oversee the response to an outbreak outside of the Ministry of Health which was managing the current outbreak and the previous ones. The new board was set up without the knowledge of the Minister who was traveling to the effected provinces at the time.
 The former Minister, Dr Oly Ilunga stated on Twitter that, “Suite à la décision de la @Presidence_RDC. de gérer à son niveau l’épidémie d’#Ebola, j’ai remis ma démission en tant que Ministre de la Santé ce lundi. Ce fut un honneur de pouvoir mettre mon expertise au service de notre Nation pendant ces 2 années importantes de notre Histoire. (Following the decision of the @Presidence_RDC to manage the # Ebola outbreak, I resigned as Minister of Health on Monday. It was an honor to be able to put my expertise at the service of our Nation during these two important years of our History.)
The former Minister, Dr Oly Ilunga stated on Twitter that, “Suite à la décision de la @Presidence_RDC. de gérer à son niveau l’épidémie d’#Ebola, j’ai remis ma démission en tant que Ministre de la Santé ce lundi. Ce fut un honneur de pouvoir mettre mon expertise au service de notre Nation pendant ces 2 années importantes de notre Histoire. (Following the decision of the @Presidence_RDC to manage the # Ebola outbreak, I resigned as Minister of Health on Monday. It was an honor to be able to put my expertise at the service of our Nation during these two important years of our History.)
 The former Minister also warned that the “Multisectoral Ebola Response Committee would interfere with the ongoing activities of national and international health workers on the ground in North Kivu and Ituri provinces.” Part of the issue may likely have been “pressure to approve a new vaccine in addition to one that has already been used to protect more than 171,000 people.” People had warned about the potential confusion to the public as well as ethical issues if a second vaccine was used, especially one that did not have the strong accumulated evidence from both the current outbreak as well as the previous one in West Africa.
The former Minister also warned that the “Multisectoral Ebola Response Committee would interfere with the ongoing activities of national and international health workers on the ground in North Kivu and Ituri provinces.” Part of the issue may likely have been “pressure to approve a new vaccine in addition to one that has already been used to protect more than 171,000 people.” People had warned about the potential confusion to the public as well as ethical issues if a second vaccine was used, especially one that did not have the strong accumulated evidence from both the current outbreak as well as the previous one in West Africa.
One might have thought that this would be a time when stability was needed since “The WHO earlier this month declared the outbreak a Public Health Emergency of International Concern, a rare step meant to highlight the urgency of the moment that has been used only four times before.” In addition, “the World Bank said it would release $300 million from a special fund set aside for crises like viral outbreaks to help cover the cost of the response.”
Unfortunately one of the msain impediments to successful Ebola control, violence in the region, continues. CIDRAP stated that. “the Allied Democratic Forces (ADF), a rebel group, attacked two villages near Beni, killing 12 people who live in the heart of the Democratic Republic of the Congo’s (DRC’s) ongoing Ebola outbreak. The terrorists killed nine in Eringeti and three in Oicha, according to Reuters. ADF has not publicly pledged allegiance to the Islamic state (ISIL), but that hasn’t stopped ISIL from claiming responsibility for the attacks.” It will take more than a change of structure in Kinshasa to deal with the realities on the ground.
 CIDRAP also observed that since the resignation of the Health Minister, “DRC officials have provided no update on the outbreak, including statistics on the number of deaths, health workers infected, or suspected cases.” The last was seen on 21 July 2019.
CIDRAP also observed that since the resignation of the Health Minister, “DRC officials have provided no update on the outbreak, including statistics on the number of deaths, health workers infected, or suspected cases.” The last was seen on 21 July 2019.
ReliefWeb reports that, “Adding to the peril, the Ebola-affected provinces share borders with Rwanda and Uganda, with frequent cross-border movement for personal travel and trade, increasing the chance that the virus could spread beyond the DRC. There have already been isolated cases of Ebola reported outside of the outbreak zone.”
These are troubling times when parasites and mosquitoes are becoming more resistant to our interventions and when governments and communities are resistant to a clear and stable path to disease containment and control.
Case Management &Resistance Bill Brieger | 22 Oct 2017
The Need to Prevent the Spread of Malaria Drug Resistance to Africa
Chike Nwangwu is a Monitoring and Evaluation Specialist who is currently working on his Doctor of Public Health (DrPH) degree at the Johns Hopkins Bloomberg School of Public Health. Here he presents an overview of the threat of parasite resistance to first-line antimalarial drugs and the need to prevent the spread of this problem in Africa which beard the greatest burden of the global malaria problem.
Malaria, remains one of the most pervasive and most malicious parasitic infections worldwide. Malaria is caused by Plasmodium parasites when they enter the human body. There are currently five known plasmodium species that cause malaria in humans- P. falciparum and P. vivax are the most prevalent globally. These parasites are transmitted through the bites of infected female anopheles mosquitoes “malaria-vectors” which perpetuate the spread of the parasite from human-human or from host- human.
Globally, according to the WHO, an estimated 212 million cases of malaria and 429 000 malaria related deaths occurred in 2015.[1] The global share of malaria is spread disproportionately across regions; Over 90% of global malaria cases and deaths occurred in the African region, with over 70% of the global burden in one sub region-Sub Saharan Africa. In areas with high transmission of malaria, children under 5 are at the highest risk to infection and death; more than two thirds of all malaria deaths occur in this age group.[2]
 Although malaria remains a global concern, malaria is preventable and curable. Increased efforts in malaria prevention and treatment within the past two decades has led to revolutionary success- 6.8 million lives have been saved globally and malaria mortality cut by 45% since 2001.[3] Globally, within a five-year interval (2010-2015) new malaria transmission and mortality in children under 5 years of age fell by 21% and 29% respectively. This has been the one the greatest public health successes in recent years [4]
Although malaria remains a global concern, malaria is preventable and curable. Increased efforts in malaria prevention and treatment within the past two decades has led to revolutionary success- 6.8 million lives have been saved globally and malaria mortality cut by 45% since 2001.[3] Globally, within a five-year interval (2010-2015) new malaria transmission and mortality in children under 5 years of age fell by 21% and 29% respectively. This has been the one the greatest public health successes in recent years [4]
The improvement of malaria indices aligns with intensification of efforts, through funding, research, innovation pushing the scale up of key malaria interventions in the malaria prevention- diagnostic- treatment cascade. For example, in Sub-Saharan Africa where malaria is most prevalent, there has been a recorded 48% increment in Insecticide Treated Net (ITN) usage since 2005, 15% rise in chemoprevention in pregnant women and within the same time frame diagnostic testing increased from 40% of suspected malaria cases to 76%.[5]
Treatment/ Emergence of insecticide and drug resistance
Malaria treatment plays a key role in controlling its transmission. First, prompt and effective treatment of malaria prevents progression to severe disease and limits the development of gametocytes, thus blocking transmission of parasites from humans to mosquitoes.[6] Drugs can also be used to prevent malaria in endemic populations, including various strategies of chemoprophylaxis, intermittent preventive therapy, and mass drug administration can be effective.[7] Like other interventions, availability and use of antimalarial has been a success. However, this has also come with some challenges. The emergence of resistance, particularly in P. falciparum and P. vivax to antimalarial-quinine and sulfadoxine-pyrimethamine, has been a major contributor to reported resurgences of malaria in the last three decades.[8]
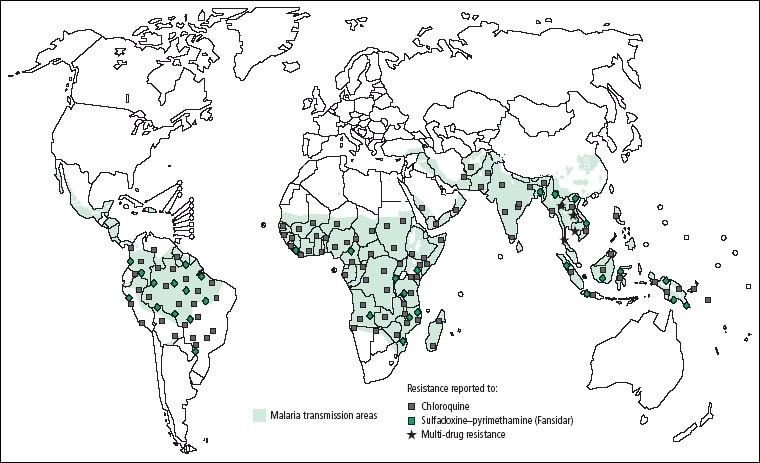
Distribution of reported resistance to antimalarials. As at 2005, antimalarial resistance was is established in 81 of the 92 countries where the disease was endemic (WHO, 2004)
Falciparum resistance first developed in some areas in Southeast Asia, Oceania, and South America before the 70’s eventually the parasite became resistant to other drugs (sulfadoxine/ pyrimethamine, mefloquine, halofantrine, and quinine. Drug-resistant P. vivax was first identified in 1989 in one region and later spread to other regions of the world.[9] As at 2005, antimalaria resistance to chloroquine and sulfadoxine-pyrimethamine was established in 81 of the 92 countries where the disease was endemic. (Figure 1) In 2005, alongside acetaminophen, antimalarial were among the most commonly abused medications in the African region, with the majority of the population having detectable amounts of chloroquine in the blood.[10]
Antimalarial drug resistance is the decrease in viability of an antimalarial to cure an infection. Parasite resistance results in a delayed or partial clearance of parasites from the blood when a person is being treated with an antimalarial.[11] Antimalaria resistance occurs as the byproduct of at least one mutation in the genome of the parasite, giving an advantageous capacity to evade the impacts of the drug. Within the human host, drug resistance develops gradually. First, a modest number of drug-resistant parasites survive exposure to the drug whilst the drug-sensitive parasites are eliminated. In the absence of additional drugs and competition from drug-sensitive pathogens, the drug-resistant parasites proliferate and their populace develops. This new population is therefore resistant to additional malaria medications of the same type.
Following the discovery of resistance to quinine and sulfadoxine-pyrimethamine, the development of resistance was initially forestalled by the utilization of a new class of malaria drugs – Artemisinin-derivative combinations. These ACTs (Artemisinin Combination Therapy) work by combining artemisinin and an active partner drug with different mechanisms of action. The WHO, with guidance from extensive drug efficacy tests and research, recommends the use of 5 types of ACTs for treatment of uncomplicated malaria caused by the P. falciparum parasite. By 2014, ACTs have been adopted as first-line treatment policy in 81 countries.[12]
Although ACT use has been a breakthrough in malaria treatment, development of resistance to de novo ACTs poses one of the greatest threats to malaria control efforts. P. falciparum resistance to artemisinin has been detected in five countries of the Greater Mekong sub-region (Lao, Myanmar, Thailand, Cambodia, and Vietnam). To date P. vivax resistance to an ACT has not been detected.
Artemisinin resistance is currently defined within the confines of delayed parasite clearance; it represents partial/relative resistance-i.e. most patients who have delayed parasite clearance do not necessarily have treatment failure. Following treatment with an ACT, infections are still cleared, as long as the partner drug remains effective. Various factors are believed to contribute to the development and spread of resistance to artemisinin; use of oral artesunate monotherapies (oAMT) inclusive.
 A global response has been mounted to curtail the spread of ACT resistance to other regions, especially to regions like Sub-Saharan Africa. Research on the mechanisms of drug resistance has steered efforts in the direction, recently the identification of the PfKelch13 (K13) mutations has allowed for a more refined definition of artemisinin resistance that includes information on the genotype. [13] In addition, stricter policies have been developed for malaria control; Therapeutic efficacy studies (TES) are conducted and used as the main reference from which national malaria control programmes determine their national treatment policy.[14] These studies help to ensure the efficacy of treatments with recommendations to ensure that these medicines are monitored through surveillance at least once every 24 months at established sentinel sites and in regions with emerging resistance, the creation of additional sentinel surveillance sites. [15]
A global response has been mounted to curtail the spread of ACT resistance to other regions, especially to regions like Sub-Saharan Africa. Research on the mechanisms of drug resistance has steered efforts in the direction, recently the identification of the PfKelch13 (K13) mutations has allowed for a more refined definition of artemisinin resistance that includes information on the genotype. [13] In addition, stricter policies have been developed for malaria control; Therapeutic efficacy studies (TES) are conducted and used as the main reference from which national malaria control programmes determine their national treatment policy.[14] These studies help to ensure the efficacy of treatments with recommendations to ensure that these medicines are monitored through surveillance at least once every 24 months at established sentinel sites and in regions with emerging resistance, the creation of additional sentinel surveillance sites. [15]
Preventing and containing antimalarial drug resistance- Recommendations to countries
As research is being done to fully understand the mechanisms of antimalarial resistance; basic recommendations to limit its spread have been disseminated.[16] First, the production and use of oral artemisinin-based monotherapy should be halted and access to the use of quality-assured ACTs for the treatment of falciparum malaria should be ensured. In countries where antimalarial treatments remain fully efficacious; correct medicine use must be promoted, with weight placed on encouraging diagnostic testing, quality-assured treatment, and good patient adherence to the treatment. Lastly, to reduce the burden of the disease, and prevent the spread of resistance, in regions where there is still high transmission, intensification of malaria control efforts is key, rapid elimination of falciparum malaria would accelerate efforts.
- [1] World Malaria Report 2016, World Health Organization, Geneva, 2016
- [2] ibid
- [3] CDC, Malaria Fast Facts 2017
- [4] ibid
- [5] World Malaria Report, 2016
- [6] Gosling RD, Okell L, Mosha J, Chandramohan D. The role of antimalarial treatment in the elimination of malaria. Clin Microbiol Infect. 2011;17:1617–1623.
- [7] Greenwood B. Anti-malarial drugs and the prevention of malaria in the population of malaria endemic areas. Malar J. 2010;9
- [8] White NJ. Antimalarial drug resistance. J Clin Invest. 2004;113:1084–1092
- [9] CDC, Malaria Fast Facts, 2017
- [10] White NJ. Antimalarial drug resistance. J Clin Invest. 2004;113:1084–1092.
- [11] Peter B. Bloland, Drug resistance in malaria, World Health Organization, 2001
- [12] World Malaria Report, 2016, World Health Organization, Geneva,2016
- [13] Artemisinin and artemisinin-based combination therapy resistance April 2017,World Health Organization, 2017
- [14] Responding to antimalarial drug resistance, World Health Organization, 2017: http://www.who.int/malaria/areas/drug_resistance/overview/en/
- [15] ibid
- [16] Ibid
Drug Development &Resistance &Treatment Bill Brieger | 06 Aug 2016
Preventing Malaria Drug Resistance in the African Setting …
… and Dealing with it Should Resistance Occur
Professor Joseph Ana, Africa Centre for Clinical Governance Research & Patient Safety in Calabar, Nigeria shares his experiences and concerns in this blog.
Drug resistance is one of the biggest challenges facing health care systems in the world today. Around 25,000 people die each year from resistant viral and bacterial infections in Europe, but no new classes of antibiotics have come on the market for more than 25 years. The figures are difficult to obtain for Africa and other developing countries.
Drug resistance is considered important in the failure of control and treatment of diseases its consequences, and it is considered to be one of the causes of emergence of new strains of infective organisms and re-emergence of once-controlled diseases. The occurrence and impact of the phenomenon is worse in Africa and parts of Asia for malaria according to WHO and the US CDC. Viral and bacterial diseases are also affected in this region.
Therefore, there is urgent need for global sustained action to prevent drug resistance from happening, and to control it, if it happens. The causes of Drug resistance are varied including lack of or poor implementation of the control of access to drugs, population migration and movement, misdiagnosis, under-treatment and irrational drug prescription and use.
 To prevent drug resistance, countries need to legislate and implement adequate control of access to drugs, sustain public education on the dangers of drug resistance, educate health workers on and enforce rational drug prescribing and use. Effective monitoring of treatment outcomes is also important to know when drug resistance is occurring. With the global and country by country best efforts drug resistance may still occur because of mutation and adaptation of infective organisms.
To prevent drug resistance, countries need to legislate and implement adequate control of access to drugs, sustain public education on the dangers of drug resistance, educate health workers on and enforce rational drug prescribing and use. Effective monitoring of treatment outcomes is also important to know when drug resistance is occurring. With the global and country by country best efforts drug resistance may still occur because of mutation and adaptation of infective organisms.
For diseases like Malaria for which resistance to the most effective drug today, artemisinin-combination drugs, is being reported from Southeast Asia, the development of new drugs alongside vector control is essential by all countries, particularly in Africa.
Professor Joseph Ana – BM.BCh (UNN), FRCSEd, FRSPH, JtCertRCGP-UK, DFFP (RCOG)-UK, DipUrology-UK, Cert.ClinGov.UK; Lead Consultant Trainer / CEO; joseph ana <jneana@yahoo.co.uk>; Contact: Africa Centre for Clinical Governance Research & Patient Safety; @Health Resources International (HRI WA); Consultants in Clinical Governance & Patient Safety (MDCN Accredited CPD Provider); 8 Amaku Street State Housing (& 20 Eta Agbor Road UNICAL Road), Calabar, Nigeria.
Visit Website: www.hriwestafrica.com; email: hriwestafrica@gmail.com Tel: +2348063600642
Elimination &Eradication &Leadership &Mortality &Resistance Bill Brieger | 29 Dec 2015
Does Malaria Meet the Criteria for Eradication?
 What it is that makes a disease “eradicable,” or more correctly what makes it possible to eliminate malaria in each country leading to the total eradication world-wide. Bruce Aylward and colleagues identified three main sets of factors by drawing on lessons of four previous attempts to eradicate diseases (including the first effort at malaria eradication in the 1950s and ‘60s).[1]
What it is that makes a disease “eradicable,” or more correctly what makes it possible to eliminate malaria in each country leading to the total eradication world-wide. Bruce Aylward and colleagues identified three main sets of factors by drawing on lessons of four previous attempts to eradicate diseases (including the first effort at malaria eradication in the 1950s and ‘60s).[1]
- biological and technical feasibility
- costs and benefits, and
- societal and political considerations
So far smallpox is the only success because as Aylward et al. pointed out biologically, humans were the only reservoir and on the technical side a very effective vaccine was developed. The eradication campaign was promoted in clear terms of economic and related benefits. While the early malaria eradication efforts started with political will and recognition of the potential economic benefits of malaria eradication, the will was not sustained over two decades. On the technical side at that time there was only one main tool again malaria, indoor residual insecticide spraying, and mosquitoes quickly developed resistance to the chemicals. Are we better able to meet the three eradication criteria today?
Today’s technical challenges are embodied in intervention coverage problems. The World Malaria Report of 2015[2] (WMR2015) explains that the problem is most pronounced in the 15 highest burden countries, and consequently these showed the slowest declines in morbidity and mortality over the past 15 years. Use of insecticide treated nets and intermittent preventive treatment for pregnant women hovers around 50%, while appropriate case management of malaria lags well below 20%, a far cry from the goals of universal coverage. A further explanation of the technical challenges as outlined in the WMR2015 lies in “weaknesses in health systems in countries with the greatest malaria burden.”
The economic benefits criteria should be most pronounced in the high burden countries, but these are also generally ones with low personal income. Ironically, the WMR2015 points out that it is the high costs of malaria care and the malaria burden that further weaken health systems. More investment is needed in order to see more economic benefits.
Biological challenges to elimination are also identified in the WMR2015. Examples of existing and arising biological difficulties include –
- Plasmodium vivax malaria which requires a more complicated regimen to affect a cure.
- “Since 2010, of 78 countries reporting (insecticide resistance) monitoring data, 60 reported resistance to at least one insecticide in one vector population.
- “P. falciparum resistance to artemisinins has now been detected in five countries in the Greater Mekong subregion.” Historically chloroquine and sulfadoxine-pyrimethamine resistance spread from this area and now artemisinin resistance marks a ‘Third Wave” of resistance emanating from the region.[3]
- “Human cases of malaria due to P. knowlesi have been recorded – this species causes malaria among monkeys in certain forested areas of South-East Asia,” and so far human-to- human transmission has not been documented.
On the positive side greater political support to elimination efforts has been expressed by the African Leaders Malaria Alliance (ALMA) who met at the African Union Leaders Summit in Addis Abba early in 2015 and resolved to eliminate malaria by 2030.[4] This call to action was backed up with an expansion of ALMA’s quarterly scorecard rating system of African countries’ performance to include elimination indicators.[5]
In conclusion, political will exists, but needs to be backed with greater financial investment in order to produce economic benefits. Time is of the essence in taking action because biological and technical forces are pressing against elimination. 2030 seems far, but we cannot wait another 15 years to take action against these challenges to malaria elimination.
[1] Aylward B, Hennessey KA, Zagaria N, Olivé J, Cochi S. When Is a Disease Eradicable? 100 Years of Lessons Learned. American Journal of Public Health, 2000; 90(10): 1515-20.
[2] World Health Organization. World Malaria Report 2015. WHO Press, World Health Organization, 20 Avenue Appia, 1211 Geneva 27, Switzerland, 2015.
[3] IRIN (news service of the UN Office for the Coordination of Humanitarian Affairs). “Third wave” of malaria resistance lurks on Thai-Cambodia border. August 29, 2014. http://www.irinnews.org/report/100549/third-wave-of-malaria-resistance-lurks-on-thai-cambodia-border
[4] United Nations Secretary-General’s Special Envoy on MDGs. African Leaders Call for Elimination of Malaria by 2030. Feb. 3, 2015. http://www.mdghealthenvoy.org/african-leaders-call-for-elimination-of-malaria-by-2030/
[5] African Malaria Leaders Alliance. ALMA 2030 Scorecard Towards Malaria Elimination, December 2014. http://alma2030.org/sites/default/files/sadc-elimination-scorecard/alma_scorecards_poster_english.pdf
Borders &Elimination &Resistance &Surveillance Bill Brieger | 29 Sep 2015
Epidemiology of Resurgent Malaria in Eastern Zimbabwe: Risk Factors, Spatio-Temporal Patterns and Prospects for Regaining Malaria Control
Mufaro Kanyangarara and her PhD thesis adviser, Luke Mullany, of the Johns Hopkins Bloomberg School of Public Health Department of International Health, have been looking into the challenges of controlling and eventually eliminating malaria in a multi-country context in southern Africa. We are sharing abstracts from her pioneering work. The first seen below provides an overview of the three components of the study.
 Despite recent reductions in malaria morbidity and mortality due to the scale up of malaria interventions, malaria remains a public health problem in sub-Saharan Africa, especially among children under five years of age, pregnant women and people living with HIV/AIDS. A recent resurgence in malaria, in areas where malaria control was previously successful, has brought to the forefront the importance of research to understand the epidemiology of malaria and the effectiveness of malaria control efforts in resurgent settings. Using cross-sectional surveys, routine data from health-facility based surveillance and freely available remotely sensed environmental data, this research examined the distribution of malaria and the impact of vector control in Mutasa, a rural district in Zimbabwe characterized by resurgent malaria.
Despite recent reductions in malaria morbidity and mortality due to the scale up of malaria interventions, malaria remains a public health problem in sub-Saharan Africa, especially among children under five years of age, pregnant women and people living with HIV/AIDS. A recent resurgence in malaria, in areas where malaria control was previously successful, has brought to the forefront the importance of research to understand the epidemiology of malaria and the effectiveness of malaria control efforts in resurgent settings. Using cross-sectional surveys, routine data from health-facility based surveillance and freely available remotely sensed environmental data, this research examined the distribution of malaria and the impact of vector control in Mutasa, a rural district in Zimbabwe characterized by resurgent malaria.
Firstly, individual- and household level factors independently associated with individual malaria risk were identified using multilevel logistic regression models based on data from cross-sectional surveys conducted between October 2012 and September 2014. Secondly, geostatistical methods and remotely sensed environmental data were used to model the spatial and seasonal distribution of household malaria risk; then develop seasonal malaria risk maps with corresponding maps of the prediction uncertainty. Lastly, an evaluation of the effect of introducing an organophosphate for indoor residual spraying was conducted using routine health facility data covering 24 months before and 6 months after the campaign.
The results of multilevel model suggested that malaria risk was significantly higher among individuals who were younger than 25 years, did not sleep under a bed net, and lived close to the Zimbabwe-Mozambique border. The spatial risk maps depicted relatively increased risk of finding a positive household in low-lying areas along the Mozambique border during the rainy season. Lastly, the introduction of organophosphates to this pyretheroid resistant area resulted in a significant reduction in malaria incidence following spraying. These findings elucidate the heterogeneous distribution of malaria, identify risk factors driving malaria transmission and assess the quantitative impact of switching insecticide classes on health outcomes. Collectively, the findings provide evidence to guide country-specific decision making for regaining malaria control and underscore the need for strong between-country initiatives to curb malaria in Mutasa District and elsewhere.
Resistance &Treatment Bill Brieger | 15 Aug 2015
Drug-resistant malaria in Myanmar: A call for increased funding to prevent a global catastrophe
We are happy to re-post a blog by Alice Sowinski, Craigen Nes, and Diane Del Pozo in the SBFPHC Policy Advocacy Blog of the Social and Behavioral Foundations of Primary Health Care Course at the Johns Hopkins Bloomberg School of Public Health….
The CDC estimates there are 198 million cases of malaria that occur worldwide with more than 500,000 people dying from the disease every year. Although this disease has slowly declined in recent years, experts believe that certain endemic areas could still be at high risk for drug resistance. One such area includes Myanmar, a Southeast Asian region located on the border between India and China.
Over 76% of Myanmar’s population lives in regions stricken with poverty and poor health infrastructure that contribute to the mass spread of disease in areas where malaria is endemic. This area in particular is becoming resistant to artemisinin, the first line of defense. Experts suggest Myanmar is a priority region for the elimination of artemisinin resistant malaria (ARM) in order to avoid the international disaster that would result if ARM were to spread to India and Africa. Immediate and large-scale action along with substantial financial support from multiple stakeholders is needed to prevent further spread of ARM and avoid a looming malaria catastrophe.
The Burmese government estimates that it will need US$1.2 billion over the next 15 years or $80 million per annum. The proposed solution would strengthen surveillance, increase rapid diagnostic testing and create new drugs to combat ARM. However, recently the Australian government, one of the 3MDG Fund donors, the largest development fund in Myanmar, has decided to cancel its pledged sum of $42 million in aid to the country. The implications of this withdrawal are uncertain and untimely.
With the ability of the malaria parasite to thwart off once effective drugs, the fear of widespread resistance is now a reality. Scientists believe we have a small window of opportunity to support Myanmar’s national campaign to increase funding to prevent a global health disaster and achieve Myanmar’s 2030 malaria elimination goals.
Asia &Borders &Resistance Bill Brieger | 25 Aug 2012
Asia-Pacific: a region of contrasting hopes for eliminating malaria
The burden of malaria in the Asia-Pacific region, being much lower than that of Africa, has led to some neglect in the past when it comes to rolling back the disease. Two news reports today show why neglect is not an option is global country-by-country elimination os the disease is to be achieved.
 Hope was expressed clearly by national Department of Health authorities in the Philippines who exclaimed that “THE Philippines could be malaria-free by 2020 as the number of cases declined by 80 percent in the recent years, the Department of Health (DOH) said on Friday.” The article in the Manila Sun-Star quoted Health Secretary Enrique Ona who said “The government has recorded 9,642 malaria cases in 2011 as compared to 43,441 in 2003.”
Hope was expressed clearly by national Department of Health authorities in the Philippines who exclaimed that “THE Philippines could be malaria-free by 2020 as the number of cases declined by 80 percent in the recent years, the Department of Health (DOH) said on Friday.” The article in the Manila Sun-Star quoted Health Secretary Enrique Ona who said “The government has recorded 9,642 malaria cases in 2011 as compared to 43,441 in 2003.”
A close accounting of the 58 provinces that are considered endemic in the Philippines found that nine have had no cases in the past three years, and forty have been reporting less than 1 case per 1000. While definitely being optimistic about the prospects of overall elimination from the country, the Health Secretary is realistic as quoted by the Sun-Times: “The journey towards elimination status is more difficult than working for a reduction in cases and we will need more commitments and resolutions of the different sectors to be consolidated into a singular, comprehensive initiative so that the whole country, not just the 58 endemic provinces, will be declared malaria-free by 2020.”
The situation in another regional partner is more dire. VOA reports that the problem of malaria drug resistance is “more severe in Cambodia than anywhere else in the world.” The National malaria Center in Cambodia found that, “About 17 percent of all cases in the Cambodian-Thai border area of Pailin were drug-resistant in 2011, up from 10 percent the year before.”
On the positive side, even though the proportion of drug-resistant cases in increasing, the total number of cases continues to decrease. Still, there is concern about ramification of the situation “beyond borders.” Travel and migration among the Mekong region countries means that resistance may not stay put in Pailin. A comprehensive control program, not just reliance on treatment, needs to be in place throughout the region.
Fortunately there are groups like the Asia Pacific Malaria Elimination Network (APMEN) that brings countries in the region together to address common and cross-border challenges. APMEN recognizes that, “Elimination requires a different strategy than sustained control,” and is thus, in am important position to help the rest of the world learn innovative approaches to put paid to malaria.
Elimination &Eradication &Resistance Bill Brieger | 08 Apr 2012
Scale-up Meets Resistance
News this week from The Lancet confirming suspicions of malaria parasite resistance to artemisinin-based drugs deals a double blow to malaria control efforts coming just a few months after announcements by Global Fund to cancel Round 11 funding. Pressure on malaria drugs is nothing new, especially since the same problem has arisen in the same region of the world for two previous and cheaper mainstays of malaria case management.
In all our hopes for rolling back malaria over the past 14 years, did we tell ourselves that such resistance was this time not inevitable?  Unlike in previous waves of resistance, this time we should have been better prepared with effective anti-vector measures. BUT this assumes that we have met our RBM targets and are happily progressing toward 2015 expecting no more malaria deaths.
We get reports that scale-up and case reduction are occurring, such as a recent newspaper article from Jigawa State in Nigeria, but basically we have not achieved our 2010 scale-up targets – so what will come first – 2015 success or the wave of parasite resistance spreading out from Southeast Asia?
The hopes of the current RBM effort were based on the fact that by 2000 we had 3-4 effective anti-malaria interventions, unlike the reliance on mainly one during the first stab at eradication. Unfortunately the question is still the same as it was in the 1950s-60s – are our health systems strong enough to deliver the goods? More effective interventions that do not reach people will not present a strong bulwark against spreading drug resistance.
 Frustration may mount even more when we realize that all the insecticide treated nets distributed over the prolonged period of campaigns from 2009-2012 will need to be replaced, mostly well before 2015. Our coverage to date has not been adequate, our funding is threatened – what guarantees that we can keep up with adequately containing malaria before the resistant strains of the parasite reach Africa where the bulk of cases and deaths occur?
Frustration may mount even more when we realize that all the insecticide treated nets distributed over the prolonged period of campaigns from 2009-2012 will need to be replaced, mostly well before 2015. Our coverage to date has not been adequate, our funding is threatened – what guarantees that we can keep up with adequately containing malaria before the resistant strains of the parasite reach Africa where the bulk of cases and deaths occur?
Some of our ‘easy’ eradication targets like guinea worm and polio are still flaunting their capacity to harm. These like other previous efforts are at risk from donor fatigue. Malaria, which is more complex than those two diseases, is at even greater risk. The RBM Partnership needs to develop a serious and workable strategy to get well ahead to the resistance wave NOW.
Asia &Resistance &Urban Bill Brieger | 23 May 2011
Mumbai – is transmission season increasing?
The Times of India reports that, “Malaria is no longer restricted to just monsoon months as in the past. Spurred on by widespread construction activity and the resulting poor sanitation, the disease has becomes a round-the-year feature in Mumbai, killing less people but afflicting more.”
An increase was noted: “In all, 76,755 contracted the ailment in 2010, 74% more than the 2009’s figure of 44,035,” but with fewer deaths (better case management?), but it is not clear whether these cases were parasitologically diagnosed.
A member of the medical association attributes the increase, especially the off-season rise, to human activity – construction projects. The official stated that, “Construction sites have puddles of water in which mosquitoes breed. Since construction work goes on throughout the year, so does the breeding. This obviously increases the incidence of malaria.”
Worry was also expressed about, “resistance developed by the Anopheles albimanus mosquito that the civic body’s insecticide fumigation has no effect on it.” This has led the city to consider using “bacillus thuringiensis variety israelensis” for control.
Ironically, in pointing out that, “Another reason for the spread of malaria, which is caused by a parasite called plasmodium, during non-monsoon months is that plasmodium can stay in the body for a long period,” the article raises the possibility that the upswing may not be fully due to new transmission.
 Aside from these possible limitations on the validity of the data, the potential for increased transmission is worrisome, especially in a part of the world that has received less (but increasing) attention from the Roll Back Malaria Partnership. The map from the 2008 World Malaria Report shows the extent of the problem in Asia.
Aside from these possible limitations on the validity of the data, the potential for increased transmission is worrisome, especially in a part of the world that has received less (but increasing) attention from the Roll Back Malaria Partnership. The map from the 2008 World Malaria Report shows the extent of the problem in Asia.
India has a double problem with malaria, hosting both P. vivax and P falciparum. A recently published article reports that while the national control program has introduced artemisinin-based combination therapy for P. falciparum as a first-line treatment, the older drugs, chloroquine (CQ) and Sulphadoxine-Pyrimethamine (SP) are still available. Unfortunately Shrabanee Mullic and colleagues found that, “In Jalpaiguri District the overall failure rate of CQ was 61% and of SP 14%, which was well above the WHO recommended cut-off threshold level (10%) for change of drug policy.”
Other research in India examined vector control with positive effects. “A study was conducted to evaluate the preventive efficacy of insecticide-treated mosquito nets (ITMNs) and mosquito repellent (MR) in a malaria-endemic foothill area of Assam, India, with forest ecosystem.” The researchers found that, “The total vector population in the three intervention sectors decreased significantly compared with that of the non-intervention one.”
Overall, malaria in India is a complex phenomenon with different forms of the parasite, different ecological settings and different levels of government involved. More attention is needed to address this complex situation is malaria is ever to be eliminated.

